Medicaid or Flat Co-Pay Insurance Plan
Set up this Insurance Plan Type when the plan pays a flat fee instead of a percentage. Insurance coverage will be 100%.
Write-offs are not tracked. To track write-offs, see HMO / DMO Insurance Plan with Co-pays.
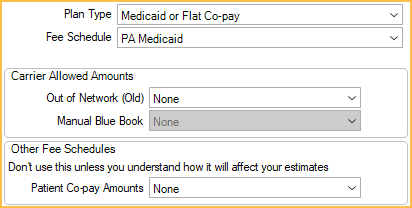
On the Insurance Plan, select these options.
- Plan Type: Medicaid or Flat Co-Pay. This will clear all percentages, maximums and deductibles, but a warning message will show first.
- Fee Schedule: The carrier's fee schedule.
- Patient Co-pay Amounts: The copay fee schedule for the carrier.
If insurance does not cover a procedure for some reason, and the office does not expect the patient to pay, enter the procedure fee as a write-off when receiving the claim.
If a patient is required to pay a copay for procedures
- Create a copay Fee Schedule for the carrier.
- For each procedure code, enter the patient's copay amount. There can be just a few fees with the rest blank. If you only have the insurance copay fee schedule, not the patient copay amounts, use this equation to obtain the fee:
Carrier Fee - Insurance Copay = Patient Copay

