Canada Claim History and ROT
For Canada users, in the Manage Module, click Send Claims.
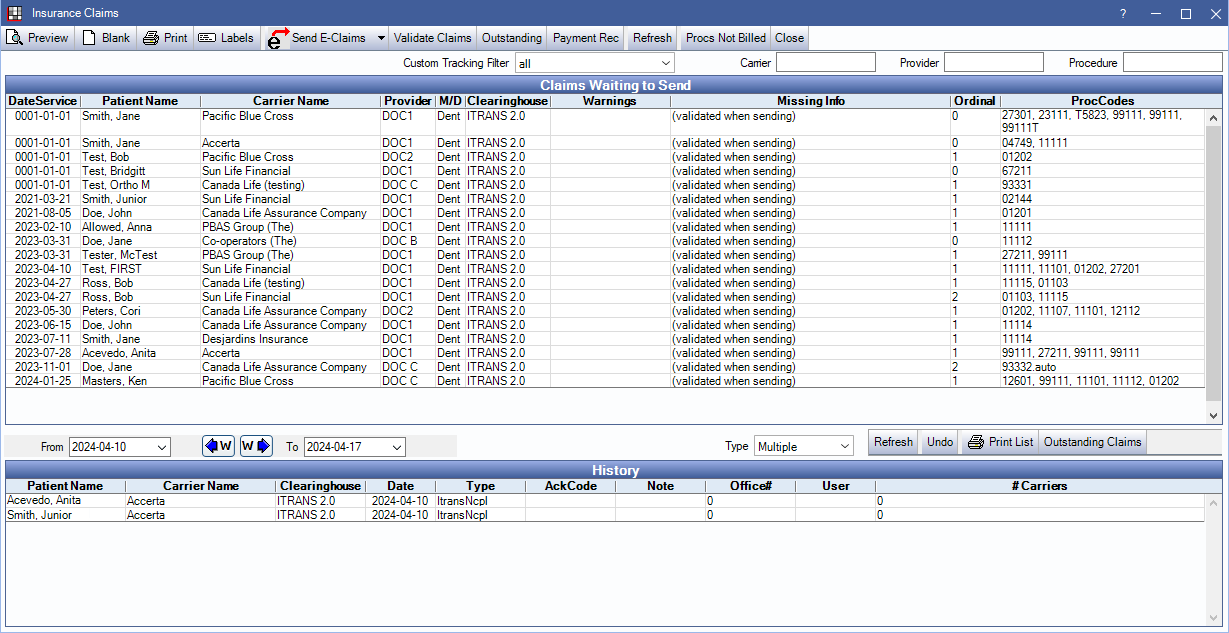
Canadian insurance claims can be managed on the Insurance Claims window. Claims cannot be sent as a batch in Canada.
For a full description of all buttons and columns, see Send Claims. Below is detail on features specific to Canada.
Toolbar
Toolbar options:
- Outstanding: Request outstanding transactions (ROT) from the default clearinghouse. See Retrieve Reports below.
- Payment Rec: Get payment reconciliation transactions for a specific carrier, billing and treating provider. This report is not used often.
Retrieve Reports (ROT - Request Outstanding Transactions)
Users are alerted of outstanding transactions (mailbox items) when sending claims. Retrieving them is optional and does not affect patient accounts.
Click Outstanding to retrieve reports.
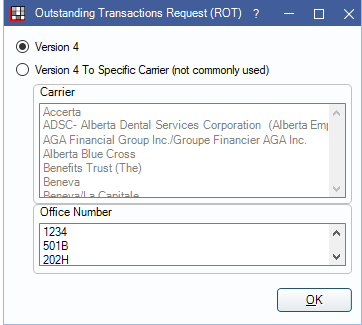
If a user is notified of outstanding transactions upon sending a claim, and would like to retrieve them, they should use these options (in any order):
- Version 4: Selected by default. Sends the ROT (04) request to recently used carriers.
- Version 4 To Specific Carrier: Select this option, a carrier from the list and the appropriate Office Number, then click OK. Useful when retrieving mailbox items immediately after receiving the notification (select the most recent carrier that a claim was sent to).
Wait for responses to show. When each step is complete, a dialog with the word Done shows.
History
Undo: Changes a sent claim status to Waiting to Send.- Does not reverse sent claims. See Reversals section in Canada Claims for more information.
- A record of sent or printed claims are available in the History grid. Double-click a row to view sent and received information.

